UI Researchers find that back braces are effective
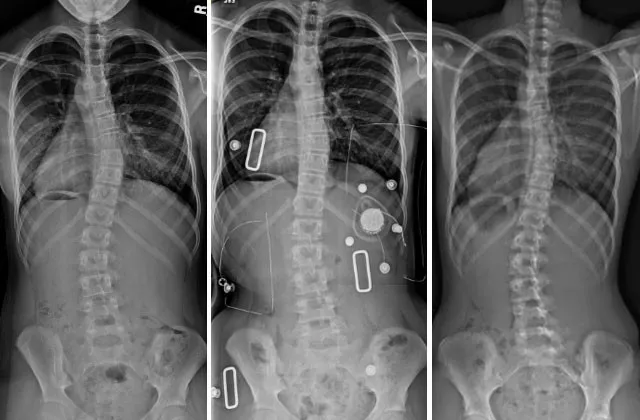
Left, an x-ray of a 12-year-old girl with scoliosis—a double curve of 28 and 23 degrees. Middle, after 4 weeks of wearing a plastic brace with metal clips, the curves measured 11 by 19 degrees. Right, after 3 years of treatment, the girl reached skeletal maturity and finished the study with curves of 14 and 20 degrees—a success. Images courtesy of UI Carver College of Medicine.
A multi-center study led by University of Iowa researchers to determine whether wearing back braces would prevent the need for spinal correction surgery in children with adolescent idiopathic scoliosis (AIS) was cut short when early results were overwhelmingly in favor of bracing.
The study was published in the New England Journal of Medicine today, Thursday Sept. 19.
Stuart Weinstein, Ignacio V. Ponseti chair and professor of Orthopaedic Surgery and professor of Pediatrics at Stead Family Children’s Hospital, and Lori Dolan, a research scientist in the Department of Orthopaedics and Rehabilitation at the UI Carver College of Medicine, led a study team that set out to compare the risk of curve progression in patients with AIS who wore a brace with patients who did not. The study team, from the Bracing in Adolescent Idiopathic Scoliosis Trial, recruited patients who were at risk for continued worsening of their spinal curves based on age, skeletal immaturity, and curve severity.
AIS is a curvature of the spine with no clear underlying cause. In mild cases, monitoring over time by a physician may be all that is needed. However, in more severe cases—especially when the child is still growing—the use of a brace, or even surgery, may be recommended. Left untreated, more serious curves can be painful and deforming.
Weinstein has been working with scoliosis patients for nearly 40 years, and although bracing has been used as a treatment for curvature of the spine since 1948, he says there has always been some question as to whether it was truly an effective way to avoid surgery.
“The efficacy of bracing was never really proven,” he says. “I wasn’t sure if braces really worked or not, and I’ve treated thousands of patients.”
He says the literature about bracing “wasn’t convincing that it worked.” Additionally, he says, some patients still required surgery after wearing a brace.
For the study, investigators enrolled 383 subjects at 25 institutions in the United States and Canada between March 2007 and Feb 2011. Although the study began as a completely randomized clinical trial, the team eventually added a “preference cohort,” where patients and families could choose their own treatment. About 40 percent of study participants were randomly assigned to bracing or to close observation without bracing. The remaining participants made their own choice regarding bracing or observation.
Patients in the observation arm received no specific treatment, while those in the bracing arm were instructed to wear a brace for 18 hours per day. Treatment was considered to be unsuccessful when a curve progressed to 50 degrees or greater—a point at which surgery is typically recommended. Treatment was considered a success when the child reached the age of skeletal maturity without this degree of curve progression.
In January 2013, the trial was stopped early after finding that bracing significantly reduced the risk of curve progression and the need for surgery, and that more hours of brace wear were associated with higher success rates. Among both the randomized and preference cohorts, 72 percent in the bracing group, and 48 percent in the observation group achieved success. In addition, the results suggest that the more a patient wore the brace, the better the results; wearing a brace more than 13 hours per day was associated with success rates of 90 to 93 percent.
“This study definitely shows braces work and are effective in preventing the need for surgery,” Weinstein says. “Children who are at risk should be treated with a brace, and they should wear it at least 13 hours a day for it to be effective.”
According to the researchers, the findings are clinically relevant to patients for whom bracing would typically have been recommended. But until now, that recommendation had not been based on solid data. “This study presents important evidence addressing the fundamental question facing families and clinicians dealing with the diagnosis of AIS—does bracing prevent the need for surgery? The answer is clearly ‘yes’,” Weinstein says.
The investigators also suggest that current bracing indications may be too broad, since 48 percent of patients in the observation group and 41 percent of patients in the bracing group who wore the brace infrequently also achieved success. “Further analysis will help us identify those AIS patients for whom bracing may be the most beneficial,” Weinstein concludes.
This release contains information from the National Institutes of Health.
This research was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases of the National Institutes of Health under Award Numbers R21AR049587 and R01AR052113.