Overview of asthma
Miles Weinberger, MD
Professor of Pediatrics
Allergy, Immunology, and Pulmonary
Common and important questions:
- What is asthma?
- Is all asthma the same?
- Why does someone get it?
- What can be done about it?
- Will it ever go away?
- Does asthma cause permanent damage?
What is asthma?
Asthma occurs because the airways in the lungs overreact to various stimuli, resulting in narrowing with obstruction to air flow. This recurrently results in one or more of the following symptoms:
- Tightness in the chest
- Labored breathing
- Coughing
- Noises in the chest heard particularly during a prolonged forced expiration (wheezing). As a result of these symptoms, asthmatics may not tolerate exertion. They may be awakened frequently at night. More severe symptoms may result in requirements for urgent medical care and hospitalization. For a very few with particularly severe asthma, there is a risk of fatality.
Asthma affects the airways, which begin just below the throat as a single tube called the trachea. The trachea is situated immediately in front of the esophagus, the passageway that connects the throat with the stomach. The trachea divides into two slightly narrower tubes called the main bronchi (each one is called a bronchus). Each main bronchus then divides into progressively smaller tubes - the smallest are called bronchioles - to carry air to and from microscopic air spaces called alveoli. It is in the alveoli that the important work of the lung occurs, exchanging oxygen in the air for carbon dioxide in the blood. The airways (trachea, bronchi, bronchioles) are surrounded by a type of involuntary muscle known as smooth muscle.
The airways are lined with a mucus membrane that secretes a fine layer of mucus and fluid. This mucus washes the airways to remove any bacteria, dirt, or other foreign material that might get into our lungs. The overreaction or hyper-responsiveness of the airways results in bronchospasm, which is excessive contraction or spasm of the bronchial smooth muscle. The airways also become inflamed with swelling of the bronchial mucous membrane (mucosa) and secretion of excessive thick mucus that is difficult to expel. It is part of the evaluation process to identify the role of each of these physiologic components in asthma. This is important because bronchospasm (constriction of the muscle surrounding the airways) and inflammation respond to different medications.
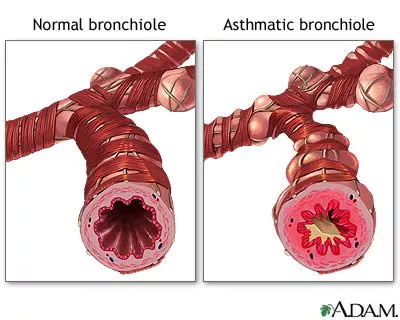
The airway hyper-responsiveness leading to obstruction of the airways occurs from one or more of various stimuli that vary with the individual patient. These include:
- Viral (but not bacterial) respiratory infections (common colds)
- Inhaled irritants (cigarette smoke, wood burning stoves and fireplaces, strong odors, chemical fumes)
- Inhaled allergens (pollens, dusts, molds, animal danders)
- Cold air
- Exercise
- Occasional ingested substances (aspirin, sulfite preservatives, specific foods). Sometimes these exposures just act as triggers of brief symptoms with rapid relief once exposure ends. Sensitivity of the airway may be increased, however, following even brief exposure to one of these. This causes a longer period of asthmatic symptoms. More information should be provided to you for each of these that are judged to be important for your asthma.
The obstruction of the airways decreases the rate at which air can flow. This is felt as tightness in the chest and labored breathing (dyspnea). The obstruction and inflammation causes coughing. Obstruction to air flow can be measured with pulmonary function tests, which can detect even degrees of airway obstruction not yet causing symptoms. Pulmonary function measurements can be an extremely valuable tool for your physician to make decisions regarding treatment.
The increased mucus in the airways stimulates coughing as the body attempts to clear the airways. The unusually thick (viscous) mucus is difficult to expel, however, resulting in continued coughing that fails to adequately expel the mucus. General irritability of the airways also causes coughing. The coughing and mucus production may cause some physicians to diagnose bronchitis. However, the term "bronchitis" simply means inflammation of the airways, and asthma causes airway inflammation. Consequently, anti-asthmatic medication, and not antibiotics, are the appropriate treatment. (Of course an asthmatic can, on occasion, have an infectious bronchitis that does not respond to anti-asthmatic medication, but this is usually viral and usual antibiotics are still not generally of any value - although there are exceptions to this generality).
Narrowing of the airway causes noises when air passes through them with sufficient speed. This typical high-pitched noise is called wheezing. Mucus in the airway causes a rattling sound called coarse crackles. Complete obstruction of some airways can cause absorption of air from the alveoli (air sacks at the end of the airways in the lungs). This causes portions of the lung to appear more dense and cast more of a shadow on a chest x-ray (this is called atelectasis). The rattling sounds or increased shadows on the x-ray are often misinterpreted as indicating pneumonia. The inappropriate diagnoses of bronchitis and pneumonia cause much unnecessary use of antibiotics, which are ineffective both for asthma in general and for most of the infections, such as the common cold viruses, that trigger asthma.
Is all asthma the same?
Asthma is quite variable. Symptoms can range from trivial and infrequent in some to severe, unrelenting, and dangerous in others. Even when severe, however, the airway obstruction is usually fully reversible, either spontaneously or as a result of treatment. This means that symptoms can be relieved, airway obstruction can be reversed, and pulmonary function can be made normal.
There are different patterns of asthma. Some people have only an intermittent pattern of disease. They have self-limited episodes of varying severity followed by extended symptom-free periods. The individual episodes are frequently triggered by viral respiratory infections (causes of the common cold). This is particularly common in young children in whom viral respiratory infections are frequent (as many as 8 to 12 per year during the toddler and preschool age group). Others have these intermittent symptomatic periods brought on by vigorous exertion, cold air, or specific environmental exposures. This pattern is intermittent asthma.
More prolonged periods of symptoms occur in people who have asthma from seasonal outdoor inhalant allergens. This may be from grass pollen on the West Coast or mold spores from molds that grow on decaying vegetation in the Midwest. Through a knowledge of the aerobiology in your area and allergy skin testing, your physician can attempt to identify whether the symptoms fit into this pattern of disease. This pattern is seasonal allergic asthma.
Some patients have daily or very frequently recurring symptoms. Although variable in severity, these patients do not have extended periods free of chest tightness, labored breathing, exertional intolerance, or cough. They may additionally have acute exacerbations triggered by the same factors that cause symptoms with an intermittent or seasonal allergic pattern of disease. Thus, viral respiratory infections (common colds) and specific environmental exposures may further increase the severity of symptoms in these patients. This pattern is chronic asthma (sometimes called persistent asthma). All patterns of disease are associated with varying degrees of severity ranging from mild to severe. It is your doctor's job, with your help, to identify the pattern and severity of disease and provide effective intervention measures to rapidly relieve acute symptoms and determine appropriate maintenance measures for those with extended symptomatic periods.
Why does someone get it?
Over 10% of people have some history of asthma. It often runs in families. The heritable nature of asthma is not well understood, however, and geneticists cannot define the precise manner in which it is passed from parents to children. All we can say is that families with asthma are more likely to have children with asthma. Although there appears to be an inherited predisposition to develop asthma, severity varies considerably among asthmatics, even among members in the same family. If asthma is present in both parents, the likelihood of a child having asthma is even greater, but even then not all of the children will have asthma. Even among identical twins, both do not necessarily have asthma, although this is more likely than if they were just siblings or nonidentical twins. This suggests that there is some additional factor that we do not yet fully understand, other than inheritance, that influences the development of asthma.
Asthma commonly begins early in childhood, even in infancy. But it can begin at any time, even among the elderly. In many cases, asthma runs in families; sometimes it does not. Sometimes it goes away with time; sometimes it does not. We do not know what causes asthma to start nor can we predict who will lose it with time. We do know that people with asthma can be provided with the means to control the disease and prevent symptoms that interfere with daily living. Rather than ask "Why do I have asthma?", it is better to ask "How can I control asthma so as to go about my usual activities without having interference from asthma?".
What can be done about it?
Asthma can be controlled. Moreover, it can be controlled by those who have asthma. The role of the physician is to provide the means for the patient to control asthma and to teach the patient to use provided measures (this is called physician-directed self-management).
Since asthma varies greatly in pattern of symptoms and severity, the treatment plan needs to be individualized. This should be done in a systematic manner. Goals of therapy must be realistically attainable and explicitly defined for you. The plan for attaining the treatment goals must be understood. Once the measures needed for control of asthma are identified, they can be placed in the hands of the patient with appropriate instructions for usage. Parental supervision is needed for young children, but progressive responsibility for self-management is given with advancing maturity.
Treatment may consist of medication, environmental changes, and life-style changes. The more the patient (or family for young children) understands the disease and its treatment, the better the outcome is likely to be. The patient (and family) should therefore be an active partner in making decisions about treatment. Be wary, however, of superstitions and misinformation regarding asthma. More than almost any other medical problem, asthma is associated with a wide diversity of medical and nonmedical opinion. Both the physician and the patient therefore need to exercise judgment. Four common sense measures to remember are:
- Ineffective measures should not be continued
- Effective measures should be continued as long as they are needed unless risk exceeds benefit
- Treatment should not be worse than the problem being treated
- Treatment should be the simplest that is adequate.
Remember that it is not sufficient just to do what is prescribed. You must also understand why measures are used so that you can be an active partner in learning what measures are required and when they should be applied. Learn the names of your medications (both the brand name and the generic name). Be critical in your observations. Report observations and concerns regarding asthma to your physician. Ask questions. Answering your questions is part of the physician's job in providing you with the skills to manage your (or your child's) asthma. The final goal is for you, not the physician, to be treating the asthma. After all, you are there when it occurs. Your physician should try to determine the most appropriate therapeutic measures. However, these measures are not optimally effective until they are implemented by you.
Will it ever go away?
Asthma has a variable course. Many children with asthma see it improve or appear to go away as they get older. This can happen any time in childhood or adolescence. If asthma was only intermittent in nature and triggered by viral respiratory infections (a particularly common form of asthma in young children), there is an excellent likelihood that asthma will be much less of a problem as the child gets older. Sometimes the nature of the asthma changes with age. A young child may have asthma initially only from viral infections. As the child ages, asthma may occur less from viral infections (because older children get fewer viral respiratory infections than younger children), but inhalant allergy may become an important contributor to the asthma. If asthma persists into adult life, or returns later in adult life after a period of remission, persisting asthmatic symptoms may not be readily explainable by any environmental factors.
Approximately half of children with chronic asthma have little or no problem after adolescence. There appears to be no way to predict who will "outgrow" their asthma and who will not. This does not relate to severity, however. Very severe asthma often goes away, and mild asthma may persist. Even when asthmatic symptoms cease to be a problem for a awhile, this is not an assurance that asthma will not return later in life. We should therefore not talk about "growing out of asthma" in children but should instead refer to extended periods of remission when asthma becomes quiescent. Asthma that persists into adult life, returns in an adult, or begins later in life, is much less likely to go into remission, although some waxing and waning of severity may occur.
Whatever the course, however, asthma is virtually always controllable with acceptably safe measures. While ongoing medical evaluation of asthma should assess whether the disease is still active and continues to need treatment, it is not wise to withhold treatment in the hope that asthma will go away by itself. That may indeed occur, but it may not, and there can be considerable avoidable suffering and disability in the interim.
Does asthma cause permanent damage?
The airway obstruction of asthma is generally completely reversible and usually does not cause permanent damage to the lungs, heart, or other organs. However, severe acute episodes of asthma can be associated with life threatening events and even fatalities. Survival of severe life threatening events can be associated with damage from lack of oxygen during the severe exacerbation, and lack of oxygen to the brain can cause loss of consciousness and brain damage.
Chronic asthma with ongoing airway inflammation may also be associated with what is called "remodeling" of the airways. This describes permanent changes occurring in the tissues surrounding the airways that results in permanent narrowing of airways. The potential for this emphasizes the importance of monitoring pulmonary function in patients with asthma at regular intervals, particularly those with a chronic pattern of asthma.
Goal of treatment - control of the disease
The primary goal of treatment is the control of asthma.
What does control of asthma mean?
- The ability to deal with acute exacerbations of asthma so that the need for urgent medical care is prevented
- Prevention of hospitalization for asthma
- Tolerating all normal activities up to and including competitive athletics if otherwise able
- The avoidance of symptoms that interfere with sleep.
- Normal pulmonary physiology (as measured by pulmonary function equipment).
- These goals should be reached safely and with the least interference with a normal life-style. The risks and bother of the treatment must be carefully weighed against the risk and bother of the asthma. The benefit obtained from the treatment must be worth any inconvenience and potential medication risks (and any medication has potential risks) imposed by the treatment.
In other words, it is the goal of treatment to determine the simplest, safest therapeutic measures that minimize disability, normalize lung function, avoid the need for acute medical care of asthma, and permit a normal life.
How the treatment goals are attained
Unfortunately, there is no magic bullet for asthma. While treatment can control symptoms safely and effectively for most patients most of the time, it is not a simple matter of the doctor writing a prescription and the patient taking the medication. Successful treatment of asthma is likely to require several steps on the part of physician. These include:
- Confirmation of the diagnosis (make sure it's asthma and not some other problem.)
- Characterization of the asthma with regard to:
- Chronicity (how frequent are the symptoms?)
- Severity (how bad do the symptoms get?)
- Identification of triggers (what makes the asthma worse?)
- Identification of the components of airway obstruction (bronchospasm, inflammation, or both?)
- Development of a plan to identify the least treatment that is safe and effective
- Teach implementation of that plan (what to do and when!)
The diagnosis of asthma is suspected when a patient has a history of recurrent or chronic shortness of breath, labored breathing, or cough in the absence of any other obvious reason. The diagnosis is confirmed by obtaining evidence that there is airway obstruction that reverses either spontaneously or as a result of treatment with anti-asthmatic measures. The procedures used to make the diagnosis include a careful history, measurement of pulmonary function (unless not practical, as in young children), and therapeutic trials of medication.
Chronicity refers to the relative persistence of symptoms and signs of asthma. Some patients have only episodic or intermittent asthma; between relatively infrequent episodes of acute symptoms, they are completely asymptomatic. Other patients have extended periods of seasonally recurring symptoms due to seasonal inhalant allergens. This pattern is classified as seasonal allergic asthma. Yet others have chronic asthma. These patients may also have brief acute exacerbations or recurring seasons of worsened symptoms but differ from intermittent or seasonal allergic asthmatics in that they do not experience extended periods free of symptoms and signs of asthma.
Assessment of severity is independent of chronicity. For any of the classifications, symptoms may range from trivial to life-threatening. Severity of acute symptoms is judged by the degree of medical care needed. Some patients never require an urgent visit to a physician or an emergency room for their asthma while others have required frequent emergency care and hospitalizations. Asthmatic symptoms that have resulted in loss of consciousness or admission to an intensive care unit identifies a particularly dangerous degree of severity.
Severity of chronic symptoms is judged by the degree of disability resulting from the daily or frequently recurring symptoms that occur in the absence of effective medication. Patients may have daily symptoms that cause only minimal discomfort. These patients tolerate activities and sleep undisturbed by their asthma. Others are literally pulmonary cripples with virtually no tolerance of activity and frequent disturbance of sleep by shortness of breath or cough.
Triggers of asthma, those identifiable factors that commonly worsen symptoms include:
- Viral respiratory infections (common colds);
- Airborne allergens (such as pollens, mold spores, animal danders, dusts);
- Inhaled irritants (such as cigarette smoke, chemical fumes, strong odors, air pollution);
- Cold air
- Exertion
Other factors can also worsen asthma on occasion. Hyperventilation, excessively rapid and deep breathing, can worsen asthma. This occurs from anxiety in some patients, particularly when asthma symptoms have begun for some other reason. A vicious cycle then occurs of asthma causing anxiety, which then worsens asthma, thereby causing more anxiety, etc. Ingested substances, such as aspirin, sulfite preservatives, and specific foods can cause acute attacks of asthma in sensitive patients.
The components of airway obstruction in asthma include bronchospasm (constriction of the muscle surrounding the airways) and inflammation. The distinction is important because the responses of each to medical treatment are different. Bronchospasm (constriction of the muscle surrounding the airways) responds to bronchodilators, medication that relaxes the bronchial smooth muscle that causes narrowing of the airway from bronchospasm. Bronchodilator medications, however, have little or no effect on mucosal edema and mucous secretions caused by inflammation. Anti-inflammatory corticosteroids (no relationship to "steroids" used by athletes to build muscle) dramatically, though slowly, reduce the mucosal swelling and mucous secretions but have no direct ability to relax the bronchial smooth muscle and relieve the bronchospasm.
An organized plan should determine specific treatment needs to control the asthma. These include medication needs, environmental alterations, and indications for allergy shots.
Medication requirements can be divided into two categories, intervention measures to relieve acute symptoms; maintenance medication to prevent the rapid return of symptoms once the intervention measures are stopped.
Patients with an intermittent pattern of asthma require only intervention measures.
Patients with sustained periods of asthmatic symptoms or asthma that returns promptly after complete clearing with intervention measures require the use of maintenance medication in addition to intervention measures.
Virtually all patients should be taught to deliver an inhaled bronchodilator to relieve or prevent acute episodes of bronchospasm. This is all that is needed for many patients. The need for corticosteroids as an additional intervention measure should be assessed based on response to bronchodilator and prior history of severity. For those with sustained periods of symptoms, maintenance medication should be selected sequentially until symptoms and signs of asthma are adequately suppressed. The goal is to permit normal sleep and activities without excessively frequent addition of intervention measures (inhaled bronchodilators and short courses of oral corticosteroids) for breakthrough symptoms.
The need for environmental alterations should be individualized as carefully as medication selection. Non-allergic irritants such as cigarette smoke or chemical fumes are usually assumed to be potentially detrimental to asthma. The use of allergy skin testing helps identify potential allergic sensitivity to specific environmental exposures. The use of allergy shots may be indicated when environmental alteration is not practical for treatment of clinically important airborne allergen sensitivity.
The treatment plan can be no more effective than its implementation. Most of the treatment, and certainly the most important aspects of the treatment, are carried out by the patient (or the family for young children). It is the physician's job (with help from other health professionals) to teach, and it is your job to learn how to carry out the treatment plan. This is an interactive and ongoing process. Use each contact, whether in person or by phone, to learn more about managing your (or your child's) asthma.