Hemorrhoids
Hemorrhoids are anal blood vessels that are a normal part of your anatomy. They can be internal—blood vessels found in the moist tissue of the inner lining of the anus. They also can be external—blood vessels found under the skin just outside the anus. Hemorrhoids can become abnormal and problematic when they become dilated or engorged. Having abnormal hemorrhoids can be referred to as hemorrhoidal disease.
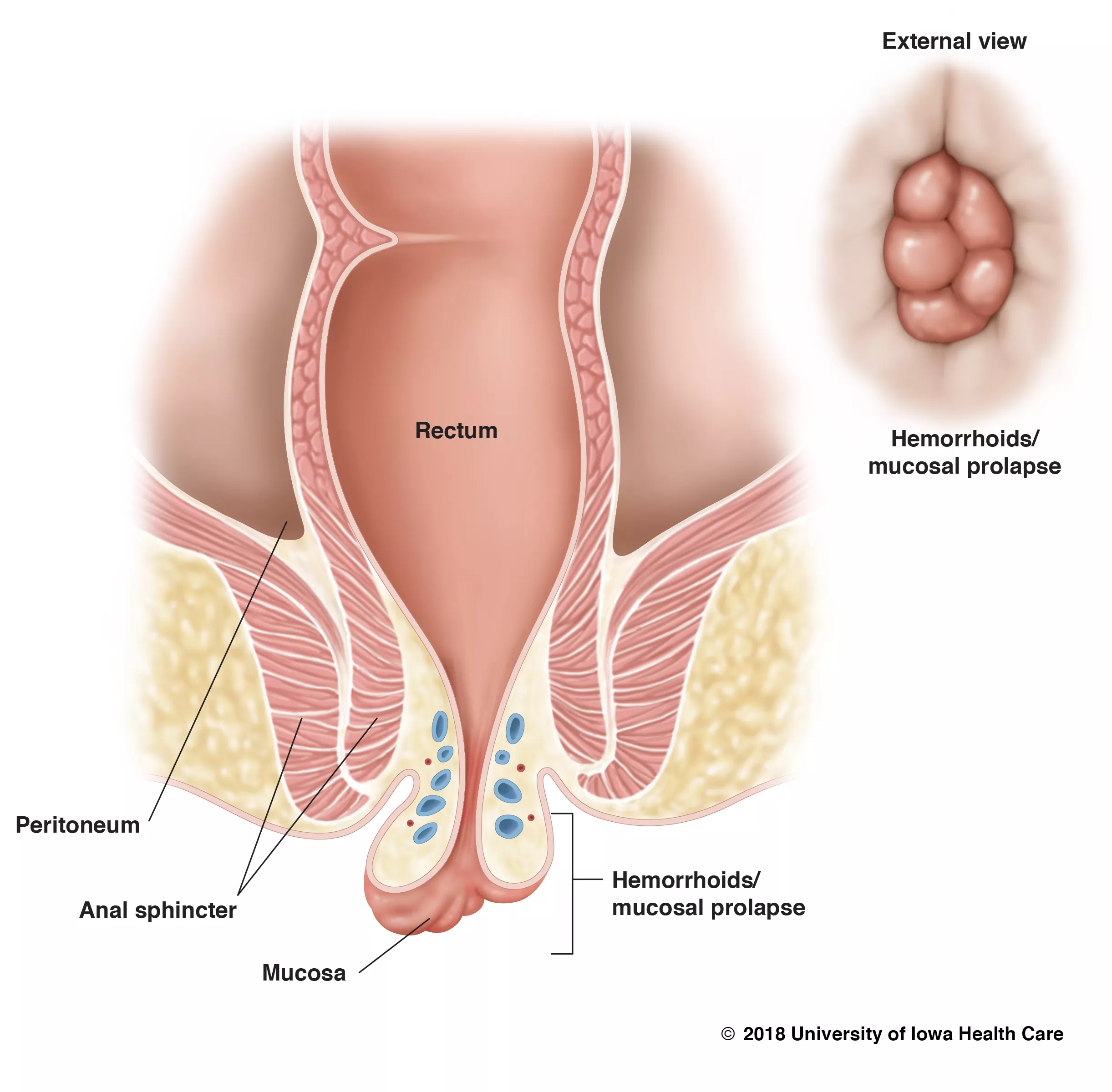
What is hemorrhoidal disease?
Hemorrhoidal disease is a common condition that occurs when your hemorrhoids become swollen due to increased pressure. This swelling leads to abnormal, symptomatic hemorrhoids. Symptoms and complications of abnormal hemorrhoids differ depending on whether the hemorrhoid is internal or external.
Symptomatic internal hemorrhoids
When internal hemorrhoids become dilated they are normally painless and associated with minor rectal bleeding and prolapse. Prolapse occurs when hemorrhoid tissue comes outside the anus while passing a stool. It is normal to feel prolapse and it is classified by four stages.
Stages of prolapse
- No prolapse.
- Prolapse that goes back in on its own.
- Prolapse that you must push back in yourself.
- Prolapse that you can’t push in yourself.
The progression of prolapse normally occurs slowly. Prolapse can irritate your anus and may cause itchiness.
Symptomatic external hemorrhoids
Thrombosed external hemorrhoids appear as a lump under the skin of the anus and can develop instantly after an episode of excessive straining. When a blood vessel is thrombosed, it means a blood clot has formed and this creates swelling. Thrombosed external hemorrhoids are typically very painful and may bleed.
After external hemorrhoids heal or the thrombosis/blood clot retreats back into the body, a skin tag may be left behind. The anus is a tightly held area and the skin covering a hemorrhoid tends to remain stretched out after the hemorrhoid is gone. Skin tags are painless, small, and almost “pinched up” pieces of skin. Although they may be bothersome, skin tags are harmless and rarely treated.
What causes abnormal hemorrhoids?
Many times, straining to have a bowel movement, constipation, or diarrhea causes abnormal hemorrhoids. Although they can also be caused by pregnancy or aging.
Who’s at risk?
Abnormal hemorrhoids tend to be hereditary. You’re more likely to get them if your parents had them. Pregnant women have an increased risk of developing abnormal hemorrhoids due to the pressure the uterus places on blood vessels in that area. The risk of developing symptoms related to hemorrhoids also increases with age.
Symptoms
The most common symptoms of abnormal hemorrhoids include:
- Itchiness
- Discomfort/irritation
- Mucus discharge
- A sense that stool is “stuck”
- Rectal bleeding
The bleeding you may experience with hemorrhoids is typically brisk, a small amount, and bright red. You may see it on toilet paper or on the stool.
How to prevent symptomatic/abnormal hemorrhoids
Follow these tips to help prevent constipation and excessive straining while passing stools.
- Eat plenty of high fiber foods.
- Drink enough water.
- Exercise regularly.
- Avoid sitting on the toilet for long periods of time.
- Use the restroom when you first feel the urge.
When to see a doctor
If you have anal pain, mucus discharge, anal itchiness, or blood in your stool, see your doctor. They can determine the cause of your symptoms and give you specific treatment options.
Diagnosis
Using one or more of the following exams, your doctor can determine if you have abnormal hemorrhoids.
Physical exam- If you have external hemorrhoids your doctor may be able to see them.
Digital rectal exam- Your doctor can insert a gloved, lubricated finger into your anus to feel for internal hemorrhoids or other abnormalities.
Anoscopy- Using a anoscope, a specialist can look for hemorrhoids or abnormalities in your anus and rectum.
Colonoscopy- This is an examination of your entire colon using a colonoscope. Similar exams may only look at the lower part of your colon, such as a sigmoidoscopy.
Treatment
Hemorrhoid treatment depends on the severity of your symptoms and state of the hemorrhoid. It is also important to treat any underlying causes of hemorrhoids, such as constipation.
At home treatments
To reduce itchiness and irritation, you can treat hemorrhoids with a warm bath with Epson salts. Ice packs can be used to reduce swelling. Adding a fiber powder to your diet and drinking more water can help ease discomfort while passing stools. Many different over-the-counter fiber powders are available. You should also consume at least 64oz of water daily and minimize caffeine. If necessary, make lifestyle changes to maintain healthy bowel habits.
Lifestyle changes
Increasing the fiber in your diet and drinking more water can ease symptoms related to hemorrhoids and help prevent them. Fiber supplements can also help soften stools. Prevent constipation by exercising regularly and consuming a healthy diet with plenty of water. If you have severe constipation or diarrhea, talk to your doctor about additional treatment options.
Hemorrhoid removal
If bothersome enough or severe, hemorrhoids can be removed by your doctor. Less than 10% of symptomatic hemorrhoids are treated with surgical removal. Removal options depend on the location and size of the hemorrhoid.
Some hemorrhoid removal options include
Rubber band litigation - A specialist places a band around your hemorrhoid that will cut off its blood flow, causing it to eventually fall off. This takes 5-7 days and you may feel slight discomfort or pressure.
Sclerotherapy - Chemicals are injected into your hemorrhoid that cause it to shrink. This procedure is typically painless but can require multiple sessions to be effective.
Infrared photocoagulation- This method uses infrared radiation (a hot light) to eliminate excess hemorrhoid tissue. It is relatively painless but may require multiple procedures to reduce your symptoms.
Hemorrhoidectomy - Surgically removing your hemorrhoid tissue can be a painful procedure with a lengthy healing time. Although, it may be an effective option for those with large symptomatic hemorrhoids.