Airway Team enhances safety for patients, staff
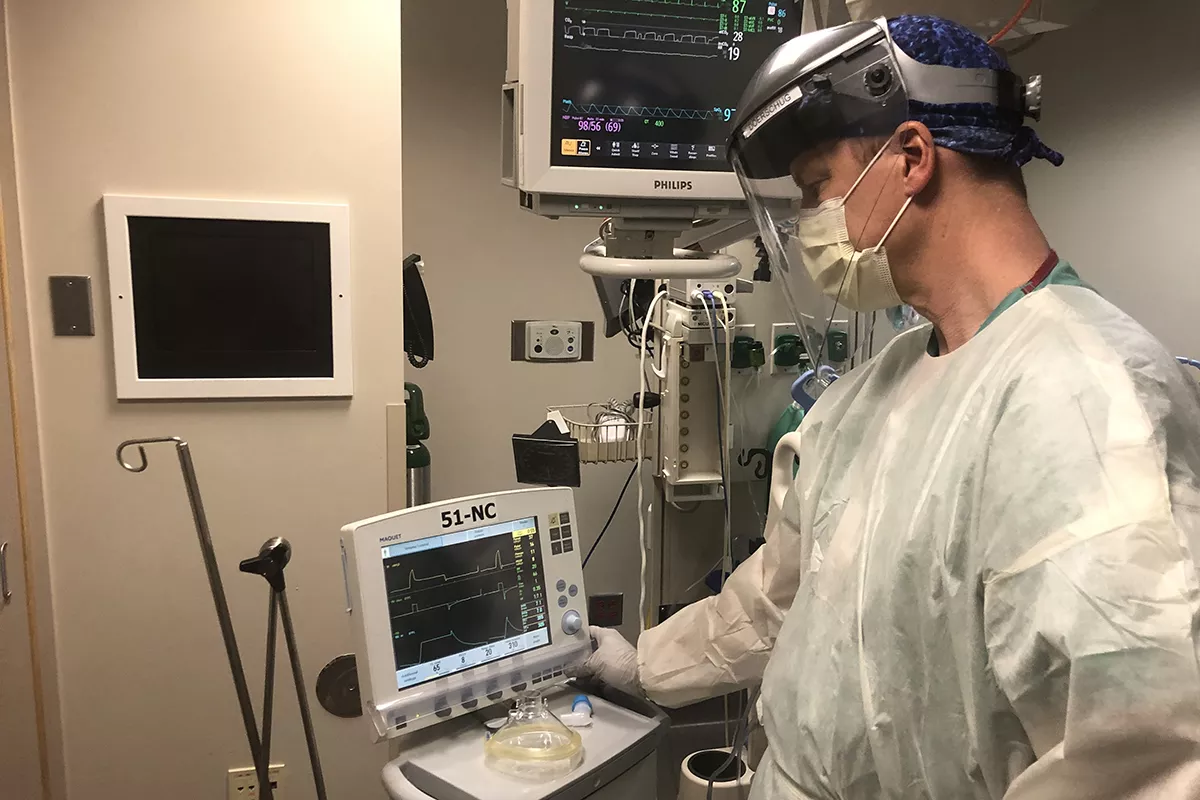
Dealing with a pandemic has challenged medical professionals to think about their work in new ways to maintain both patient and staff safety. At University of Iowa Hospitals & Clinics, one significant change has been the creation of an Airway Team whose members are responsible for all intubations for patients with COVID-19.
Melinda Seering, clinical associate professor of anesthesia and clinical director of the Ambulatory Surgery Center, led the formation of the team, which includes nurses, respiratory therapists, pharmacists, certified registered nurse anesthetists, and faculty and residents from anesthesia, emergency medicine and internal medicine—pulmonary, critical care and occupational medicine.
Before the pandemic it was common practice for six or seven medical staff to be in the room for an intubation, Seering said. However, working in such close contact with a patient’s airway carries a high risk of exposure to the virus. The goal was to reduce the number of people in the room to create a safer environment for all involved.
“At the formation of this crisis we had to sit back and decide how many people we need in the room to safely care for the patient,” Seering said. Three was the minimum number they decided upon—an airway specialist, a nurse, and a respiratory therapist. Outside the room and in constant communication via two-way radio are a second airway specialist, who is in full protective equipment in case the in-room team needs additional assistance, another nurse, and a pharmacist.
With that established, Kevin Doerschug, clinical professor of internal medicine - pulmonary, critical care and occupational medicine and medical director of the Medical Intensive Care Unit (MICU), began running simulations to ensure that everyone on the team understood their role as well as the roles of other team members. “We ran a dozen different simulation sessions to go through protocols, creating a check list, and simulating in real time so we had already practiced before seeing real patients.”
Nikki Wiltfang, assistant nurse manager for the MICU, said the simulations were invaluable in ensuring that everyone was on the same page and knew what to do. She said the nursing team decided that the charge nurses would be the ones at the bedside while the patient’s own nurse remained outside the room delivering medicine via a pump and responding to any other needs as they arise.
Seering said limiting the number of people at the bedside and limiting the pool of people participating in intubation of patients with COVID-19 enhances safety for both patients and staff. Fewer staff are exposed to the virus and those staff working with patients are the most experienced and in sync with each other, able to anticipate each other’s actions and responses.
“The number one benefit is an overall sense of calmness during intubation,” Doerschug said. “Everyone in the room and outside the room has infinite shared situational awareness, knows what’s is supposed to happen or when things are changing course. When people are acting calmly, they make better decisions.”
Wiltfang said it was a challenge for the nursing staff to have their usual workflow “turned upside down,” but they have continued to adapt and improve processes for the benefit of their patients. “We have to work as a team a lot more, finding new ways to communicate” she said, including the two-way radio between inside and outside the patient room and writing with dry-erase markers on the windows of patient room doors.
“I’ve worked in MICU 11 years, this really the biggest change to our workflow,” Wiltfang said. “We are all learning right now and adapting every single day. It’s a challenge, but so rewarding to see everyone step up and work together. As a team, everyone is holding each other up.”
Over a span of five weeks, the Airway Team was responsible for intubation for over four dozen patients with COVID-19. Intubation is used for only the most critically ill patients with COVID-19 and allows a ventilator to do the work of the lungs, delivering oxygen and removing carbon dioxide, so the lungs can rest and recover from the disease.