Iowa leads research in how measles spreads
Patrick Sinn, PhD, University of Iowa associate professor of pediatrics and microbiology and immunology, has been studying how measles infects humans since he was a graduate student at Iowa almost two decades ago.
In various studies, including collaboration with colleagues at Mayo Clinic, Sinn’s work has shown how the virus enters the body via immune system cells in the airway. These measles-infected immune cells then ferry the virus across the epithelial barrier and on to the lymph nodes. From there, the virus spreads through the body. The last cells to be infected are the airway epithelial cells before the virus leaves the host and infects the next person.
Surprising research results

“There’s a lot to know about this very successful pathogen,” Sinn says. “For example, why measles is so contagious is still an unanswered question.”
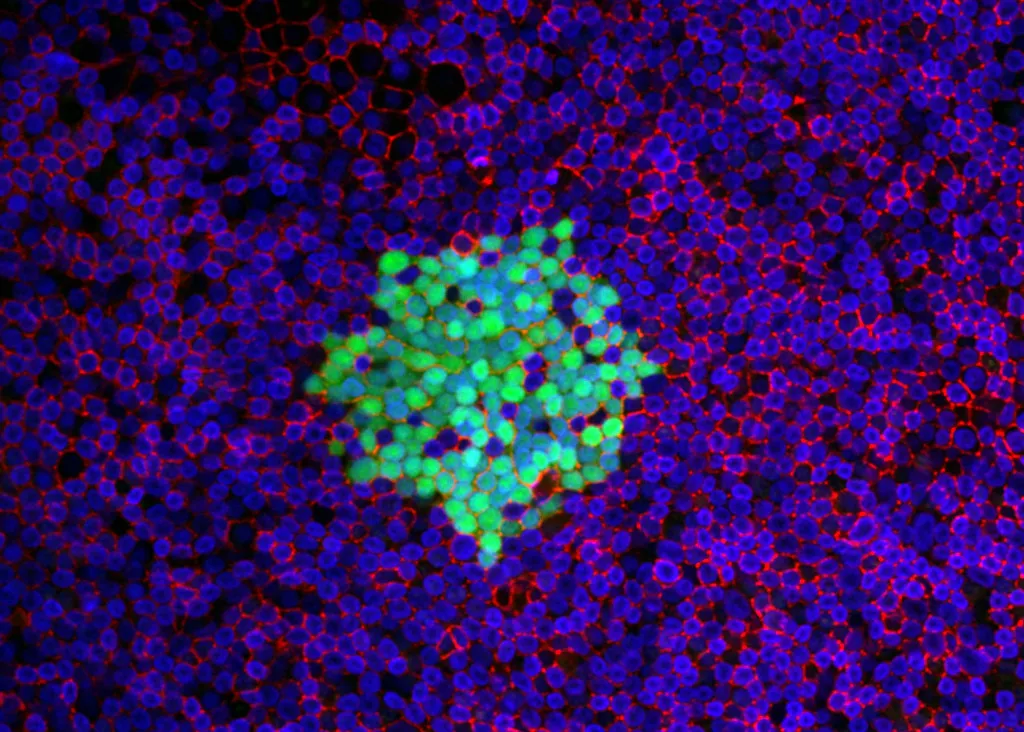
In his more recent studies, Sinn’s lab has shown that once the measles virus is inside airway cells it spreads rapidly from cell to cell. This sideways spread through the epithelial layer creates blooms or patches of infected cells that Sinn terms infectious centers. Sinn’s team, including Cami Hippee and Brajesh Singh, PhD, is investigating the role infectious centers play in the disease’s super ability to escape from the host and infect others.
“I’m convinced the infectious centers are important, and this work could suggest a new paradigm for how measles can spread from person to person,” Sinn says.
Measles on the rise
This year the United States is experiencing its worst measles outbreak since 2000, when the disease was declared to have been eliminated. The Centers for Disease Control and Prevention (CDC) reports more than 800 cases in 2019 already, compared to less than 400 in 2018.
According to the CDC:
- Measles can cause blindness, deafness, and brain damage.
- Statistically, as many as two in every 1,000 cases of measles may result in death.
- Young children, especially infants, are most vulnerable to the severe effects of the disease.
- On average, one person with measles will likely infect 12 to 18 non-immune people. Compare that with the flu virus, where two to five others may be infected, or smallpox, where five to seven others may be infected.
- An infected person sheds the measles virus for days before they show symptoms.
- The airborne measles virus can survive for several hours after it has been expressed through coughing or sneezing.
- Measles has been observed to wipe out immune memory for other pathogens, so you can lose immunity you’ve already acquired from vaccination or from having had a disease.
- Vaccination rates for measles in some parts of the country have dropped below the 95 percent needed to keep the disease in check.
On these findings Sinn says: “In some ways the success of the vaccine has created the problem where people have forgotten how deadly measles can be. If the virus infects everyone and 0.1 or 0.2 percent die, that’s still a lot of deaths. In this case, prevention is better than treatment, so whatever can be done to convince people to get vaccinated is critical. But, anything we can learn about how the virus spreads could help in the future.”