A new solution to N95 respirator fit testing
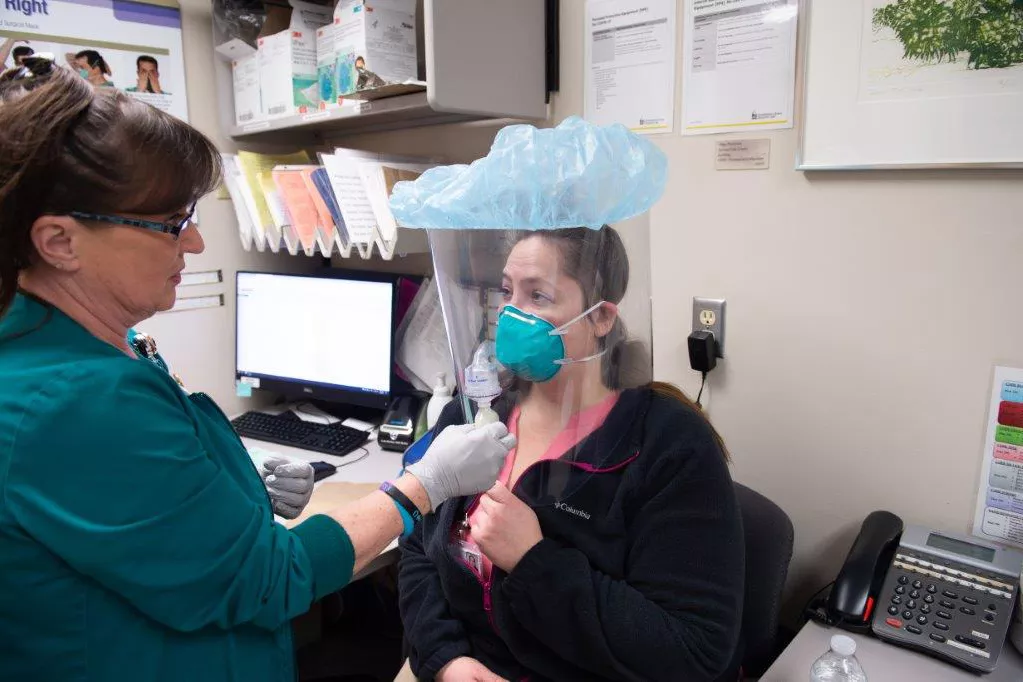
When our University Employee Health Clinic needed a different way to conduct N95 respirator fit testing, a colleague stepped up to help, implementing a solution to help conserve our PPE.
As the COVID-19 pandemic escalated in early March, our University Employee Health Clinic (UEHC) began doing more N95 fit testings, preparing additional staff to treat potential patients with COVID-19.
To ensure a proper respirator fit, staff at the UEHC were using what’s called a quantitative process. The individual being fit with a respirator would don an N95 mask, a member of UEHC would help adjust it, and then attach it to a machine that measured the dust both inside and outside of the respirator to ensure the fit was correct. The N95 respirator used in this test would then be discarded, rendered unusable after the fit testing due to a hole being punched in the respirator to allow it to hook to the machine.
Under normal circumstances, this method worked just fine. However, during a global pandemic facing global supply shortages, every effort counted to extend the life of this important piece of personal protective equipment for our employees.
That’s where Justin Newnum came in.
A sweet and bitter solution
In early March, Justin Newnum received a call to lend his expertise to staff at the UEHC. Newnum, an industrial hygienist who specializes in chemical and noise exposures at part of the University of Iowa Environmental Health and Safety department, was no stranger to N95 respirator fit testing. In fact, he and his team used a slightly different method during testing, a qualitative process, to keep staff elsewhere across the university safe.
During this qualitative process, the individual being fit with the mask would don the N95 respirator, in addition to a clear hood. An aerosolized mist with a sweet or bitter solution would be then pumped into the hood. If the individual undergoing fit testing could taste either solution, the respirator would need to be adjusted, or a different style or size would be tried.
Why use this qualitative method? The N95 respirators used in this method could be reused outside the testing process, saving us more respirators to be used by our employees.
Training our teams
Newnum jumped into action, spending time with staff at the UEHC to train them on the process. After about a week, enough UEHC staff had been trained on the process, and Newnum was able to return to his normal role.
“It feels good to be able to do what you can to help during these times,” says Newnum. “I’m proud to play a part in protecting those who care for others.”