Back on her feet despite all odds
Margaret Coleman says doctors at University of Iowa Health Care performed a miracle after she was pinned under her car, crushing her pelvis and dissociating her spine. But her doctors say she’s the one who deserves the credit.

After spending 45 minutes pinned under her car, Margaret Coleman was warned she may never walk again. Or if she did, it would only be short distances with a walker.
Eighteen months later, Coleman walks unassisted—only needing a walker for long journeys.
“She is a remarkable story,” says J. Lawrence Marsh, MD, an orthopedic surgeon at University of Iowa Hospitals & Clinics. “And the truth is, it’s her as much as anything we’ve done for her. To say, ‘I’m not just going to live, I’m going to walk again’—she is a remarkable, tough lady.”
Coleman, 81, says she feels blessed to have a full life again, crediting the expertise of all the doctors, nurses, and physical therapists she met along the way.
“I had the best care that money can’t buy,” Coleman says. “When I needed something, I had the best of the best. It must have been the Lord looking out for me because it really was true.”
On June 11, 2021, the Waukee, Iowa, resident made what was supposed to be a quick trip to the grocery store. As she started the car to return home, she noticed a grocery cart rolling toward her. She isn’t sure if she failed to put the car in park or if she knocked it out of park when she got out to grab the cart, but however it happened, the car rolled, knocking her over and pinning her underneath.
Emergency crews brought in heavy equipment to lift the car off her and took her to a Des Moines hospital, where a trauma team stemmed the bleeding and assessed her injuries.

Coleman’s sister, Kathy Evans, says the family didn’t realize initially how serious those injuries were.
“When we first saw her, she looked great and was talking,” Evans says. “But the doctor in the ER explained that it was bad and that she would need to go to Iowa City.”
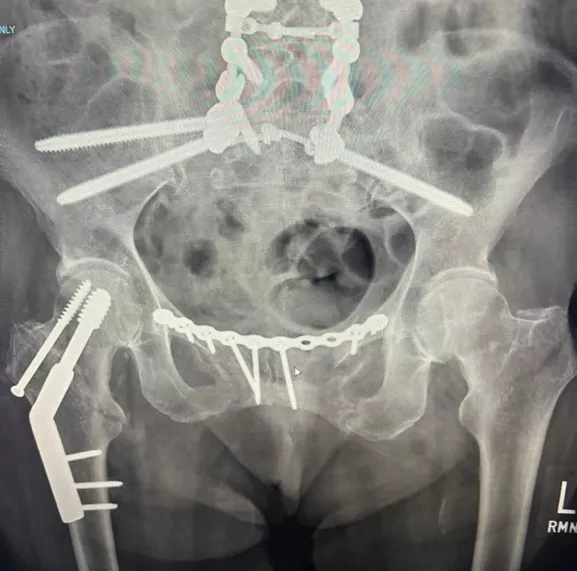
Coleman’s right femur was broken in multiple places, her left leg was open to the bone, her pelvis was crushed, her hip broken, and her spine had separated from her pelvis. She was flown to UI Hospitals & Clinics, where she underwent two major surgeries.
Marsh says perhaps the biggest challenge in Coleman’s case was her age.
“Patients her age who have a simple fall and break their hip have a 20% chance of dying over three to six months,” Marsh says. “But you add her age and a high-energy accident where you not only break your hip but dissociate your spine from your pelvis—the truth is we were worried that she wouldn’t survive surgery.”
Coleman remembers the doctors explaining that the second surgery to rebuild her pelvis and stabilize her spine would be high-risk, but she and her family decided to go forward with it.
“My daughter told me that I am the strongest person she knows, and she knew I could do it,” Coleman says. “When they took me down to surgery, Dr. Marsh wheeled me down and talked to me all the way. I don’t think that happens very often, where the surgeon actually takes the patient to the operating room. It was just so kind.”
Marsh says severe pelvic fractures generally are treated by repositioning the bone fragments into their normal alignment and holding them together with screws or metal plates. But because the pelvis was also dissociated from the spine, additional work was needed. Orthopedic spine surgeon Andrew Pugely, MD, reattached the spine and built a cage to protect it.
“By fixing metal rods and bars to the spine, we can help hold the pelvis into position,” Pugely says. “These are specialized techniques that have been used more frequently in the last decade.”
Three weeks later, Coleman returned to Des Moines, where she did rehabilitation for three months.
The doctors didn’t want her to put weight on her pelvis for at least 60 days, at which point Coleman had X-rays done in Des Moines and sent to UI Hospitals & Clinics.
Marsh says while they always like to see their patients in person, it’s not always possible due to challenges such as distance or a person’s health.
“There’s no question that telehealth has improved since COVID,” Marsh says. “It especially helps patients like Margaret because it decreases the need for transfer while still facilitating care.”
Marsh and his colleagues liked what they saw on Coleman’s X-rays.
“They said I could try to stand. So that first day I stood for about three seconds,” Coleman says. “The second day I took a step with the walker. The third day I took several steps. I knew at that point that I would work as hard as I could work to get as far as I possibly could get and I’d be happy with whatever the result was.”
In January 2022, Coleman convinced her physical therapist that she was ready to try walking unaided.
“Within the next week, I was walking without my walker—just a few steps at first, but walking,” Coleman says. “They never thought that was going to happen.”
Today, Coleman has only one quibble about the care she received: “I think Dr. Marsh made my pelvis a little bigger than it was, so I had to get different pants!”
But in all seriousness, Coleman says she is truly grateful for the care she received at UI Hospitals & Clinics.
“A surgeon I once worked with said that good health care is 60% high tech and 40% high touch, and I got exactly that every time I needed something,” Coleman says. “I would really just like to hug and thank Dr. Marsh and Dr. Pugely. I was lucky enough to get the best of the best.”
She also says she wouldn’t be where she is now without her family.
“They were a huge, huge part in helping me not just recover, but live,” Coleman says.
As for Marsh, he insists that it is Coleman who deserves the praise.
“Compliments to our team and Dr. Pugely’s team. This was a badly injured skeleton and it was put back together really well,” Marsh says. “Those are the things that we do, but most people don’t do what she’s been able to do. It’s Margaret Coleman who has done an amazing thing.”
Patient Stories

