Saved by surgery
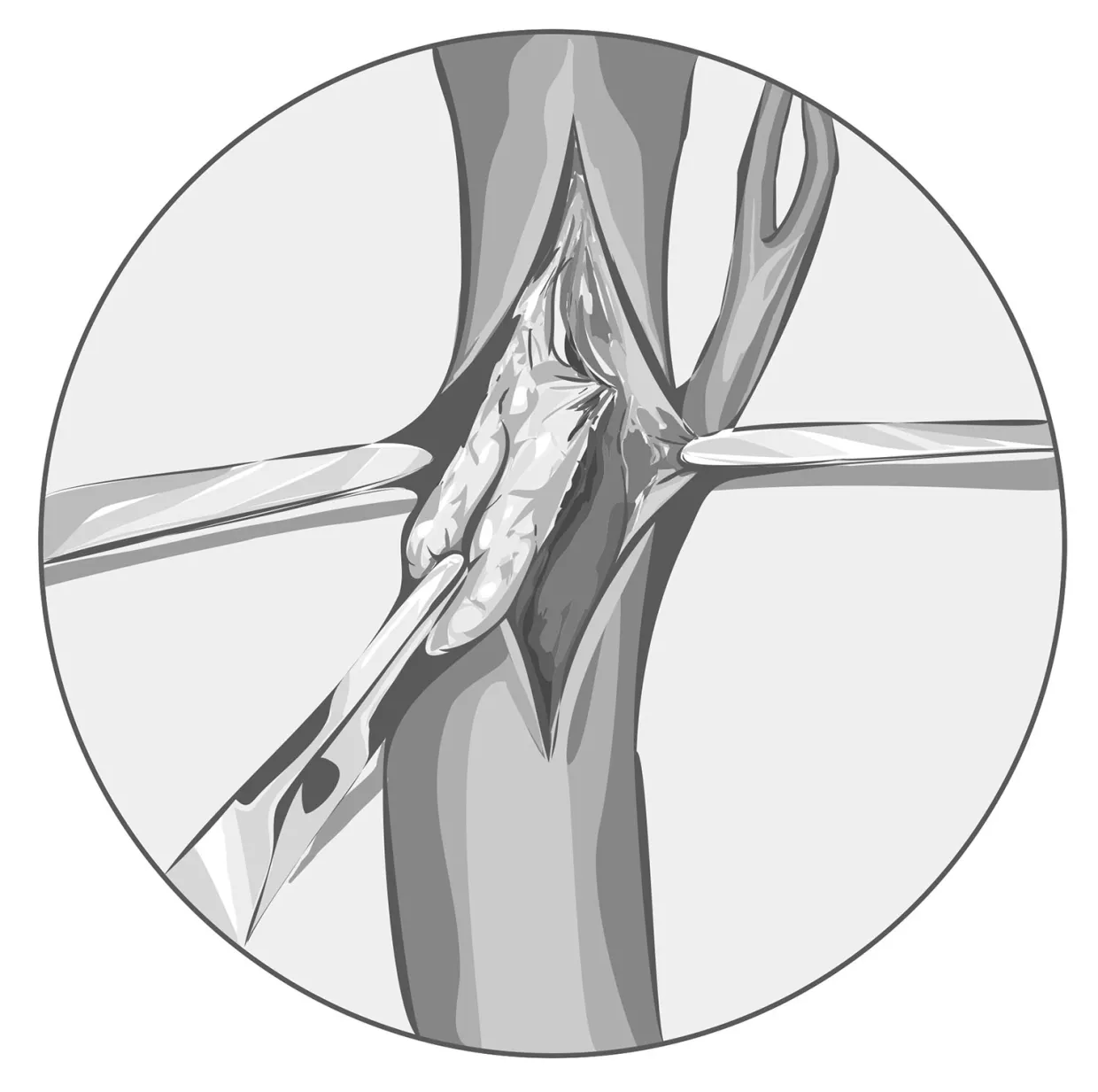
A type of pulmonary hypertension, CTEPH can be cured but is often undiagnosed
With the patient in suspended animation, her body temperature at 18 degrees Celsius (64 degrees Fahrenheit) to stop blood circulating, former University of Iowa cardiothoracic surgeon Jay K. Bhama, MD, delicately removed the clot blocking the pulmonary artery. Then the real work began as he painstakingly stripped out the inner lining of the affected blood vessel, 2 to 3 inches at a time, right down to the narrowest branch points in the lung.
The surgery—known as pulmonary thromboendarterectomy (PTE)—proceeds sequentially: Circulation is halted. The surgeon removes a section of diseased blood vessel lining. Blood flow is restored. Repeat until all the lining is removed. For approximately two hours, Bhama peeled away the inner layer of the blood vessels, pausing occasionally to let blood flow resume.
“You have to work fast during circulatory arrest because there is no blood flow to the brain. We depend on the low temperature to protect the brain. We usually try to limit that pause to 20 minutes,” Bhama explains.
This highly specialized and intense surgery can provide a cure for patients with chronic thromboembolic pulmonary hypertension (CTEPH), a rare, life-threatening form of high blood pressure in the lungs caused by blood clots.
Only a few medical centers in the nation perform PTE, which requires a coordinated team of highly skilled surgical and medical specialists to care for the patient during the procedure and through recovery.
Shortness of breath, fatigue are symptoms
CTEPH is a rare condition—about 5,000 Americans are diagnosed annually—and the symptoms are vague. Patients typically experience shortness of breath and fatigue, which can be indicators of many diseases, meaning CTEPH often goes unrecognized.
CTEPH is caused by small blood clots traveling to the lung, where they can block arteries. Often these clots, known as pulmonary emboli, are reabsorbed by the body, but in CTEPH they persist, restricting blood flow and causing pulmonary blood pressure to rise. This high pressure forces the heart to work harder to push blood through the lungs. Over time, this exertion weakens the heart muscle, leading to heart failure and premature death.
One of the most important and somewhat surprising discoveries about the pathogenesis of CTEPH is that simply removing the clot is not sufficient to eliminate the disease. The condition damages the lining of the blocked vessel, requiring removal of this innermost layer to ensure a cure.
About 3 percent of people who have pulmonary emboli will develop CTEPH, but more than half of people eventually diagnosed with the condition have no history of pulmonary embolism.
“You just really have to be suspicious of the possibility of CTEPH,” says Linda M. Cadaret, MD, director of the UI Heart and Vascular Center’s Pulmonary Hypertension Program. “It is a rare disease, but it’s important to identify it because this surgery can be curative.”
CTEPH diagnosed with lung imaging
Diagnosing CTEPH requires specialized lung imaging, including ventilation/perfusion scans (V/Q scans) that assess blood flow throughout the lungs and are the recommended screening method for CTEPH. Pulmonary angiograms or CT scans can confirm blockage of the lung vasculature and show the extent and location of the clot, and an echocardiogram can reveal right ventricular enlargement indicating heart damage caused by CTEPH.
CTEPH can affect anyone. Cadaret notes that she has cared for men and women of all ages with the condition. Anything that increases the likelihood of blood clots can increase the risk for CTEPH, including prolonged inactivity, smoking, being overweight, pregnancy, certain cancers and heart disease, as well as blood-clotting disorders like lupus.

Bhama wants primary care providers to consider CTEPH in patients who have otherwise unexplained shortness of breath and fatigue.
“My concern is that many people in Iowa are not diagnosed because there is poor recognition of the problem,” he says. “Primary care providers, general cardiologists, and pulmonologists often are not aware or do not make the connection that this could be chronic thromboembolic disease.”
Bringing specialty care to Iowans
A board-certified thoracic surgeon, Bhama specializes in advanced cardiac surgery. He is section chief for adult cardiac surgery and surgical director of cardiac transplant and mechanical circulatory support with UI Health Care. His first exposure to the PTE procedure came during fellowship training in Pittsburgh.
To deepen his understanding in preparation for providing PTE at the UI, Bhama observed and learned the nuances of the procedure from specialists at the University of California in San Diego, who pioneered the technique and have the nation’s largest and longest-running program. Previously, UI patients who were candidates for the surgery were referred to UC San Diego or the Cleveland Clinic, another well-established center. However, patients sometimes do not have the resources or support to travel so far from home.
For Bhama, serving patients locally is an important responsibility for the state’s only academic medical center. In addition, he was convinced that UI Health Care already had much of the essential infrastructure and expertise in place, including a nationally recognized comprehensive pulmonary hypertension center, directed by Cadaret, and exceptionally strong critical care support.
“There is a tremendous pool of talent here in Iowa in our hospital in so many different areas: anesthesia, critical care medicine, cardiology, and pulmonary medicine. So we really had only to add the surgical piece that was missing,” Bhama says. “Adding that gives us a really solid team, and patients will have great confidence to get their care here.”
First surgery in Iowa
On May 3, 2018, Bhama performed the first PTE in Iowa on Melisa Coburn, 29, of Vinton, Iowa.
The surgery and recovery involve an extended hospitalization, and staying close to her family was an important factor in Coburn’s decision to have the surgery at the UI.
The procedure was a success. Coburn’s pulmonary blood pressure and oxygen saturation level have normalized, and she can be more active. She lost 60 to 70 pounds, which allowed her to come off diabetes medications. Cadaret’s team continues to manage her blood-clotting condition and prevent future clots.
“Fixing this problem has helped her enjoy much better health and improved her quality of life tremendously,” Bhama says.
“We feel very fortunate that our first procedure went so well, but we don’t want to make assumptions or become overconfident. We are an early-stage program, and we will continue to look to the bigger, well-established programs for guidance. We want to really do our homework well so that we can provide the highest quality of care for our patients,” he says.