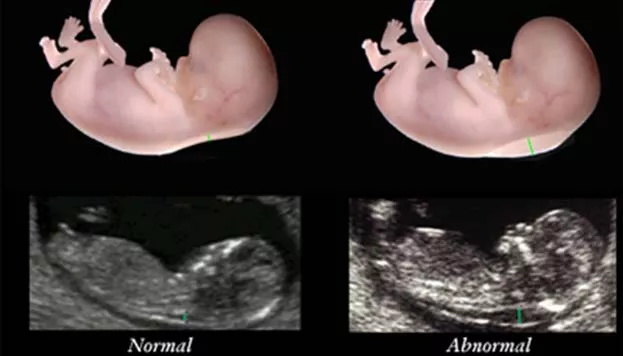
Fetal Heart Program
The fetal heart program at University of Iowa Stead Family Children’s Hospital works closely with families whose children have been diagnosed with a heart defect before birth.
For all requests:
1-888-573-5437