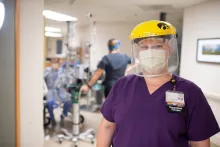
Neurological Rehabilitation
For all requests:
1-800-777-8442
Neurological rehabilitation at University of Iowa Health Care encompasses comprehensive evaluation and treatment of individuals with movement problems due to disease or injury of the nervous system. The goal of treatment is to help individuals achieve a more independent lifestyle. Therapists determine appropriate assistive devices and adaptive equipment to aid in activities of daily living. We serve a wide variety of conditions and ability levels. Our physical and occupational therapists coordinate care to meet the needs of the individual.
Common Conditions Treated Include:
- Stroke
- Traumatic Brain Injury
- Parkinson's Disease
- Multiple Sclerosis
- Spinal Cord Injury
- Muscular Dystrophy
- Neuropathy
- Balance Disorders
- Huntington's Disease
Related Clinical Care
Our Care Team
Not sure which Neurological Rehabilitation provider is right for you?
When you call 1-800-777-8442 we'll help you find a provider who meets your needs.
Locations and Offices
1701B John Pappajohn Pavilion (JPP)
Elevator J, Level 1
Resource Office

200 Hawkins Drive, Iowa City, IA 52242
2007 Roy J. Carver Pavilion (RCP)
Elevator E, Level 2
Clinic
200 Hawkins Drive, Iowa City, IA 52242
2701 Prairie Meadow Drive, Iowa City, IA 52242

701 W. Forevergreen Road, North Liberty, IA 52317

500 E. Market St., Iowa City, IA 52245
September 10, 2025
UI physical therapy professor shares tips to help you stay healthy and active
June 4, 2025
Advanced physical therapy techniques aren’t only for collegiate and professional athletes. Find relief and strength with expert physical therapy.Consu...

Patient Stories
April 13, 2026
Lynette Marshall and Jeffery Ford demonstrate generosity, love, and gratitude after transplant surgery at UI Health Care

September 30, 2015
Brent Wightman was able to get his life back after suffering from back pain from years of hard work. All thanks to the many rehabilitative services th...
Related News
July 30, 2020
Senior occupational therapist Danielle Burmeister commits to helping COVID-19 patients recovery through strengthening the body and the mind.