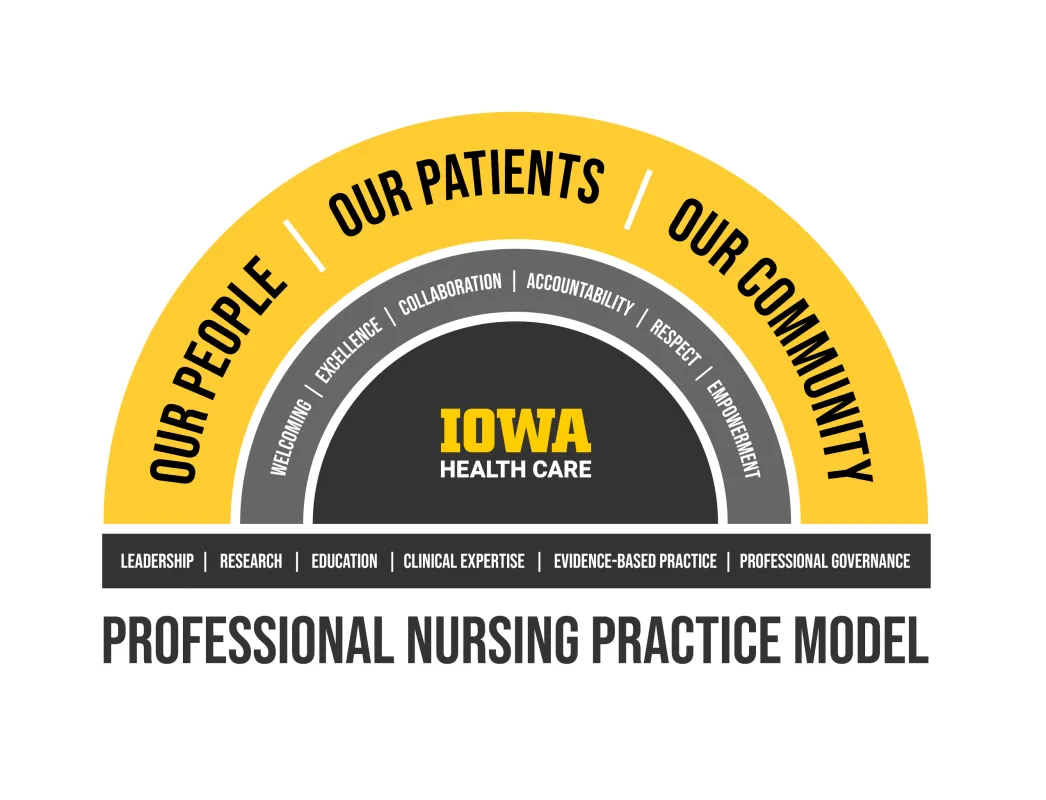
The Professional Nursing Practice Model for the Department of Nursing Services and Patient Care is a visual representation of the values, organizational structures, and processes that provide a unifying framework for nursing practice at the University of Iowa Health Care.
The model ensures consistency in the delivery of nursing care and defines for all registered nurses their authority, autonomy, and accountability as they care for patients and families in our community, state, region, nation, and the world.
Authority: the recognition and use of rights and responsibility to use nursing knowledge, skills, and judgments to provide high-quality outcomes for patients
Autonomy: the making of independent nursing decisions about the best nursing practices to provide safe, high-quality outcomes for patients
Accountability: the acceptance of responsibility for actions, judgments, and the resulting outcomes
The Elements
Foundation
The foundation represents our culture of accountability, continuous learning, innovation, and collaborative decision-making among nursing professionals. These practices are the operational investments we make that enable us to live out our values.
Through transformational leadership, our staff nurses are empowered to be leaders of patient care at the bedside. Our nurse leaders are key to the success of this practice model. They are highly visible and accessible. The chief nurse executive (CNE) is a member of the UI Health Care Clinical Systems Committee (CSC, executive advisory board). The CNE advocates for nurses throughout the health care system. Our leadership prioritizes succession planning and mentoring to ensure the continuity of nursing administration, goal achievement, and fostering of future nursing leaders.
Research, an integral component of our nursing practice, drives innovation, clinical decision-making, and advances in health care. Our nurses generate knowledge through conduct, collaboration, and participation in research practices that improve patient outcomes.
Our nurses work in an environment of continual learning. We educate and empower patients and families to understand illness and treatment, supporting them as they make health care decisions. Patient education is provided using health literacy and plain language principles.
We promote and support all professional education levels, including a nurse residency program, experienced nurse fellowship program, and ongoing professional development. The nurse residency program facilitates transition into practice and competency-based orientation. This program is accredited by the Commission on Collegiate Nursing Education. The experienced nurse fellowship program helps experienced nurses transition to acute care staff nurse roles. The American Nurses Credentialing Center accredits this program as a Practice Transition Accreditation Program. We support the pursuit of advanced degrees, professional certification, and continuing education. We participate in active role modeling, share our expertise, and learn collaboratively with colleagues across disciplines.
Collegial relationships with the UI College of Nursing and other UI health science colleges enhance the educational component of the practice environment.
Nurses are grounded in the science and art of nursing. They have exemplary clinical knowledge and the skills to provide excellent care tailored to each patient's unique needs and attributes. We work in a culture of safety and quality and utilize care-delivery models that allow nurses to be accountable for their practice and clinical decision-making at the point of care. We work skillfully in an environment with a high level of electronic information systems that support patient, family, and interprofessional communication. Engagement in the development of information systems and device integration is a key to success.
Our nurses improve the quality of care by applying new knowledge and innovations as they provide evidence-based care. We are committed to an environment that fosters scientific inquiry, critical thinking, and innovation. We support evidence-based policies, procedures, and standards of care. As internationally recognized leaders in EBP, we remain at the forefront of innovation. We support a staff nurse internship to expand EBP across the organization and provide ongoing training opportunities for nurses throughout the state, region, nation, and world.
Our nurses share decision-making responsibilities at the unit, division, department, and organizational levels through a professional governance structure dating back to 1975. All levels of our nursing staff participate in councils and committees through this structure. We are members of hospital advisory committees; we participate in unit-based committees; we help design unit-based care-delivery models; and we participate in unit-based interprofessional care councils, sharing decision-making responsibilities.
Core
The core, the center of the image, identifies UI Health Care and our collective mission and vision.
Changing Medicine. Changing Lives.
As Iowa’s comprehensive academic health system, UI Health Care:
- Provides high-quality primary and specialty care to patients and families across Iowa and throughout the region
- Teaches and trains the next generation of physicians, biomedical scientists, and health care professionals
- Seeks research discoveries that advance understanding of human health and disease and lead to new therapies and treatments
- Offers programs and services to communities that address identified health needs and provide measurable improvement in health care access, health status, and use of health care resources
To be among the nation’s best in medical education, biomedical research, and patient care toward improving the health and well-being of Iowans and their communities.
Middle Arc
The fundamental values of UI Health Care are rooted in the core: Welcoming, Excellence, Collaboration, Accountability, Respect, and Empowerment. These values define our culture, guide our daily interactions, and shape the spirit of all our ambitions.
We have an environment where everyone has a voice that is heard; that promotes the dignity of our patients, trainees, and employees; and allows all to thrive in their health, work, research, and education.
We achieve and deliver our personal and collective best in the pursuit of quality and accessible health care, education, and research.
We collaborate with health care systems, providers, and communities across Iowa and the region as well as within our UI community. We believe teamwork—guided by compassion—is the best way to work.
We behave ethically, act with fairness and integrity, take responsibility for our own actions, and respond when errors in behavior or judgment occur.
We create an inclusive environment where every individual feels safe, valued, and respected, supporting the well-being and success of all members of our community.
We commit to fair access to research, health care, and education for our community and opportunities for personal and professional growth for our staff and learners.
Outer Arc
This collective effort culminates in an expansive, outward reach, directing our priorities toward Our People, Our Patients, and Our Community. Through this model, we look toward the horizon, committed to our nursing vision: to be a destination for safe, high-quality, evidence-based nursing care, clinical education, and innovation for Iowa and the world.
Additional resources for nurses
Looking for more information about a nursing career with UI Health Care? View our resource pages to learn more.

Join our team
UI Health Care is always looking for dedicated nurses to join our team. Don’t wait—apply today to launch a meaningful career at Iowa’s top hospital.
Locations and Offices

Awards and Recognition
